MRIs were performed for clinical purposes either during an acute neurological presentation or for follow up. All patients were given intravenous gadolinium-based contrast media. Sagittal T1, T2, STIR and axial T1, T2 weighted images were obtained through the spine without contrast followed by sagittal and axial T1 weighted images obtained after gadolinium administration. Small field of view axial and coronal T2WI with fat saturation and fat saturated post contrasted axial and coronal images were obtained for orbital evaluation. For brain MRI, sagittal T1WI, axial fast spin-echo T2WI, axial/sagittal fast spin-echo FLAIR, and in some cases sagittal 3D FLAIR images, axial diffusion and ADC mapped images followed by post-contrast axial and coronal T1WI were analyzed. 
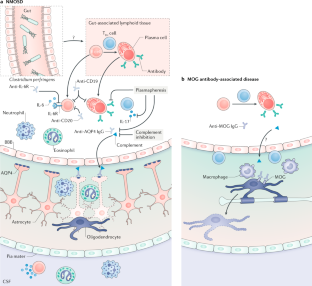
The MR exams were performed with different scanners at either 1.5T or 3T magnetic strength: Philips Healthcare (Best, the Netherlands), GE Healthcare (Milwaukee, Wisconsin), and Siemens (Erlangen, Germany). inflammatory attack(s) of the optic nerve, spinal cord or brain, including the brainstem and area postrema attacks ( 2).Īll MOG positive patients were included (n=26) and 25 AQP4 positive patients with matching age and sex were collected from the records.Īll subjects provided consent to participate in this study, which was approved by the Johns Hopkins University institutional review board. AQP4 antibody seropositivity by ELISA( four patients were tested subsequently using cell-based assay due to negative ELISA results despite strong clinical suspicion) 2. Inclusion criteria for AQP4 seropositive NMOSD were based on the 2015 International Panel on NMOSD Diagnosis which requires 1. We did not necessarily exclude patients who also met criteria for multiple sclerosis (MS) as there is no consensus-based distinction between MS and MOGAD. inflammatory attack(s) of the optic nerve, spinal cord or brain. MOG antibody seropositivity by live cell-based assay with IgG1 secondary antibody from the Mayo Medical Lab, Quest Diagnostics or the Oxford University Neuroimmunology Laboratory (UK) and 2. Inclusion criteria for MOG antibody disease were: 1. This is a retrospective analysis of patients recruited in person from the Johns Hopkins Hospital NMO clinic between 2015-2018 or recruited remotely through review of records by the principle investigator (ML). The goal is to confirm known MRI features or identify new ones in NMOSD that can prompt serological testing for the MOG antibody. In this study we retrospectively reviewed the MR imaging findings of MOG and AQP4 antibody seropositive NMOSD and compared our findings with those that have been reported. Conus medullaris is a frequent target of attack in MOGAD patients compared to the cervical and thoracic spinal cord in AQP4 NMOSD ( 13). Despite the fact that 50% of MOG patients relapse with transverse myelitis ( 7, 11, 12), they are less likely to experience cord necrosis or atrophy as a sequelae, relative to AQP4 patients ( 13– 15). Longitudinally extensive optic nerve lesions are common in both MOGAD and AQP4 seropositive NMOSD, ( 9, 10) while posterior nerve segment and chiasmatic involvement appears to be more unique to AQP4 NMOSD ( 10). MRI is instrumental in distinguishing NMOSD from multiple sclerosis (MS), but initial MR reports in MOG antibody disease identified both overlapping and unique features compared with AQP4 NMOSD ( 5, 8). Compared to AQP4 seropositive patients, MOG antibody disease (MOGAD) is thought to more commonly affect young Caucasian males, with a relatively better long-term clinical outcome ( 6, 7). Among NMOSD patients who test negative for the AQP4 antibody, up to 42% test positive for an antibody against myelin oligodendrocyte glycoprotein antibody (MOG) ( 4, 5). ( 2) Up to 87% of NMOSD patients harbor a serological antibody to the aquaporin-4 (AQP4) water channel ( 3). In 2015, the spectrum was defined to include 6 core features namely, optic nerves, spinal cord, area postrema, brain stem, diencephalic structures and cerebral hemispheres. 
It was thought to only involve the optic nerves and spinal cord leading to blindness and paralysis ( 1). Neuromyelitis optica spectrum disorder (NMOSD) is rare autoimmune central nervous system (CNS) disease.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
